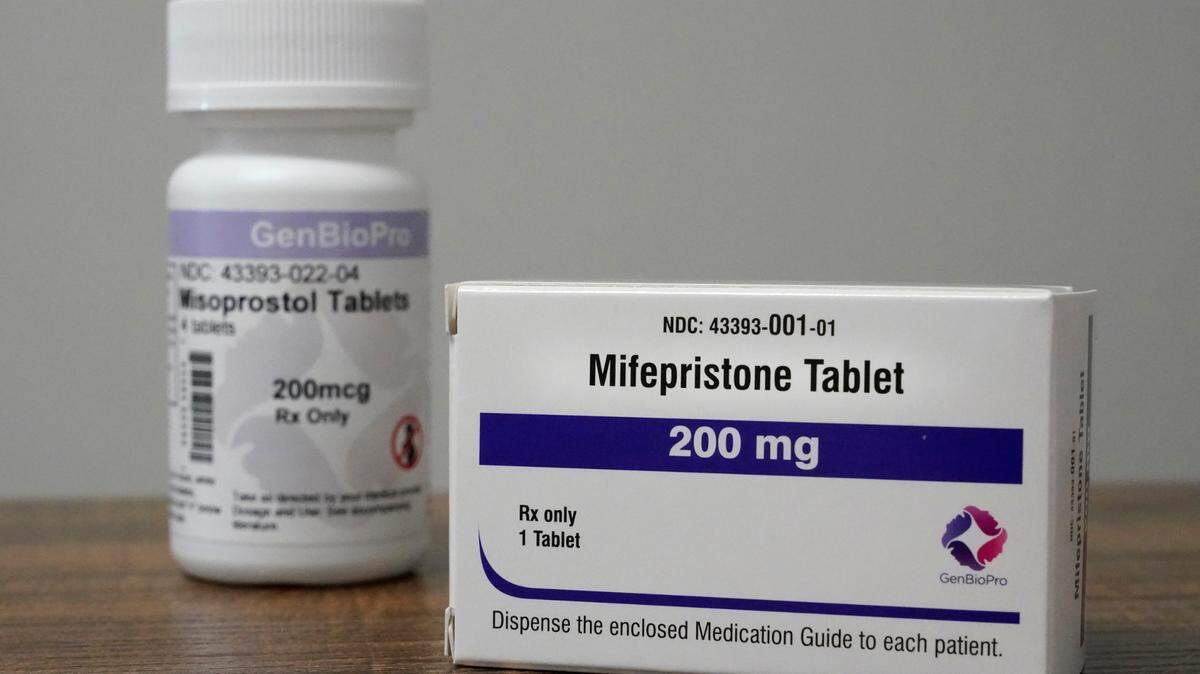
With Roe v. Wade struck down, could treatment for miscarriages suffer? Experts worry
READ MORE
What does overturning Roe v. Wade mean for KS, MO?
Kansas and Missouri now have more control over abortion access in their state following the Roe v. Wade, a landmark 1973 court ruling that established abortion as a constitutional right. Here’s what that looks like.
Expand All
This story was updated after the Supreme Court decision Friday morning.
The Supreme Court decision on Friday overturning Roe v. Wade could have a ripple effect on health care for women who aren’t trying to seek an abortion, experts say.
Doctors providing abortion care use skills and drugs similar to those used to treat miscarriages and stillbirths.
Medical residents who sign up for abortion training learn skills they use in non-abortion care, such as how to work with patients experiencing emergencies and how to clear the uterine lining to prevent dangerous complications after a miscarriage — also a method used in surgical abortions.
In the United States, most surgical abortions are performed by OB-GYNS. Nearly half of their residency programs could be prohibited from offering abortion training now that Roe v. Wade has been overturned.
If doctors aren’t trained in “non-urgent, more routine abortion care,” they might not have the skills to save a woman experiencing a life-threatening pregnancy loss, said Dr. Alhambra Frarey, professor of obstetrics and gynecology at the University of Pennsylvania and graduate of the University of Kansas School of Medicine.
“I think that this is a side of the story … that a lot of people don’t understand.”
Anywhere from 10% to 20% of known pregnancies, and likely more, end in miscarriage, defined by the Centers for Disease Control and Prevention as the loss of a baby before the 20th week of pregnancy. A stillbirth is a pregnancy loss after 20 weeks.
In a recent survey of OB-GYN residents, many in programs without abortion training felt significantly less prepared to offer care for a patient experiencing early pregnancy loss. The survey results were published in January by the American Journal of Obstetrics & Gynecology.
Researchers worried that less-prepared residents might lack the confidence to offer an emotionally stressed patient every appropriate treatment option. And when residents weren’t required to have abortion training, they were less likely to say they planned to provide comprehensive care in early pregnancy loss.
“Abortion training is already hard to get for many residents around the country, and it’s only going to get worse with Roe hanging in the balance,” wrote Dr. Sarah Horvath, lead author on the paper.
“This research shows the widespread collateral damage of these abortion restrictions for patient access to competent miscarriage care.”
Nearly 44% of the 286 accredited OB-GYN residence programs in the United States are in states certain or likely to ban abortion after Roe is overturned, according to an April analysis in the Obstetrics & Gynecology journal.
That would immediately leave 2,638 of more than 6,000 OB-GYN residents certain or likely to have no access to in-state abortion training, the survey said.
“If a resident doesn’t have training in abortion, they will receive training in miscarriage management, but it is usually less comprehensive, especially when it comes to later procedures, like in the second trimester,” said Frarey.
“A miscarriage at that stage of pregnancy is not a common outcome, so the number of procedures for pregnancy loss that any trainee would have a chance to learn from is small.”
With the Supreme Court’s decision, Missouri is set to enact a “trigger law” banning most abortions.
Kansans will have their say on abortion rights in August when they vote on a constitutional amendment that would allow the Legislature to further restrict or ban abortion. How will that affect abortion training in the state?
The Star asked medical schools in Kansas and Missouri about the abortion education they provide students and residents. Only two responded.
“It’s not possible to predict how changes in the laws in Kansas may affect our program until we know exactly what changes are proposed,” said Kay Hawes, spokeswoman for KU’s School of Medicine.
The school’s OB-GYN residency program is required by a national accrediting group to provide access to abortion training, though residents can choose to opt out.
‘Glaringly absent’ from medical school
Both the American College of Obstetricians and Gynecologists, the nation’s leading professional organization of OB-GYNs, and the American Medical Association consider abortion an essential part of reproductive health care. Both oppose limiting access.
Abortion opponents, however, do not consider abortion to be health care and say those who call it that are playing word games. “Abortion is not health care” has become a recent rallying cry as opponents work to get it banned.
They say training has been mainstreamed into residency programs to recruit doctors who perform the procedure and to normalize abortion as health care.
The CDC says there were 630,000 abortions in 2019, up slightly from the two previous years. That’s twice the number of emergency appendectomies performed in the United States every year.
“Yet abortion-related topics are glaringly absent from medical school curricula in the USA with half of medical schools including no formal training or only a single lecture,” wrote researchers at Stanford University in 2020 who studied abortion training.
Medical school students typically spend four years learning general medicine and patient care, then move into more intense hands-on training in specialized residency programs.
The abortion education mandate that applies to accredited OB-GYN residency programs does not apply to medical schools. Students who want that training often join organizations such as Medical Students for Choice, which supports and advocates for future abortion providers, or have even created lectures and workshops of their own for like-minded colleagues.
The Stanford researchers found that medical students “face a lack of educational opportunities in abortion care” compared to OB-GYN residency programs.
“The improvements made by standardizing abortion education in OB-GYN residency should encourage similar efforts in medical school in order to increase earlier and wider exposure to future physicians of all specialties,” they wrote.
“On a national level, standardizing exams for medical students by which to evaluate their understanding of abortion care would hold schools accountable for medical student education.”
‘Profound public health implications’
Did Roe v. Wade giveth and taketh away?
In a 2013 study about the ”unintended consequences” of Roe v. Wade, researchers noted how abortion care quickly shifted from hospitals to non-hospital clinics after the 1973 decision.
That made abortion more widely accessible to women, increasing the number of places they could get an abortion and other family planning services.
But it also moved the procedure, those patients and training opportunities away from hospital-based teaching programs for medical school residents.
In 2017, 95% of the abortions performed in the United States happened in outpatient clinics, with 3% performed in hospitals and slightly more than 1% in doctors’ offices, according to the Guttmacher Institute, a research and policy group that supports reproductive rights.
After Roe v. Wade, training in family planning grew increasingly uncommon in OB-GYN residency programs, researchers noted, and by the early 1990s, only 12% of residency programs in the country offered training in abortion care.
In 1996, as training dropped, the Accreditation Council for Graduate Medical Education began requiring OB-GYN residency programs to provide abortion training or allow residents to train elsewhere, away from their schools.
Accredited programs must provide access to abortion training, but residents can opt out. Despite that requirement, about 8% of residents in a 2020 study reported they had no access to abortion training.
The accreditation council is exploring alternative ways to train doctors should abortion become illegal in more states. Virtual abortion training that doesn’t include hands-on lessons is one consideration.
“Almost half of all American women will seek an abortion in their lifetime, and thus the lack of training for physicians may have profound public health implications,” wrote the researchers who studied the Roe v. Wade aftermath.
“The decades of unrelenting harassment of physicians have ensured that abortion is still a procedure that most doctors will perform only under the guise of anonymity for fear of professional and personal consequences.”
Still a stigma
The hurdles are numerous. OB-GYN residents who want the training report having to crawl through administrative red tape about malpractice insurance and licensing. The OB-GYN group has identified other roadblocks:
▪ Lack of public funding and other restrictions on medical schools and teaching hospitals that limit abortion education and training. Within the past year, bills seeking to limit abortion education have been proposed or enacted in at least eight states, the Associated Press reported.
▪ More hospitals run by churches that prohibit abortion. For instance, in 2016, 1 in 6 acute-care beds in the United States was controlled by a Catholic hospital – an increase of 18% since 2001. Providers in Catholic hospitals are required to follow church directives that prohibit abortion and many other reproductive services, such as contraception.
▪ Opt-in abortion training. Residents who want the training must seek it themselves “outside of required curricular frameworks,” the national OB-GYN group says. “It further stigmatizes it, and prevents future doctors from being able to give the best possible care to their patients,” the group says.
In a 2017 blog posting on the website of Medical Students for Choice, a sixth-year medical student at the University of Missouri-Kansas City wrote that during her OB-GYN clerkship “we delved into pregnancy, contraception, gynecologic disorders, and spontaneous abortion, but there was no discussion of elective abortion.
“When I asked faculty members about this omission they just said, ‘It’s not something we discuss.’”
UMKC, like most schools in the region, did not respond to The Star’s request for comment on abortion training.
What about local schools?
At KU’s school of medicine, “medical students receive a good working understanding of comprehensive reproductive health care, just as they receive a good working understanding of cardiac care or pediatric care,” said Hawes, the school’s spokeswoman.
“Through lectures and case studies, students in medical school receive a foundation of learning, not a foundation of procedures.”
Students at Washington University School of Medicine in St. Louis receive information about abortion in two lectures over their four-year education, said spokeswoman Judy Martin Finch.
Both KU and Wash U. said they follow the accreditation council’s requirement that their OB-GYN residency programs offer residents training or access to training in abortion. At both schools, residents can choose not to participate.
When it came to getting clinical experience in abortion care, “I remember seeking it out, I don’t remember it being something that was really openly broadcast as an opportunity,” said Frarey, who completed medical school and residency at KU 10 years ago.
“I was fortunate that when I started my residency at KU Med, there was a wonderful faculty member there … and she wanted as part of her work at KU to spend a little time at our local Planned Parenthood providing early abortion care.
“So in my, I believe it must have been my first year of residency, I was allowed to go for four, half-days with her to Planned Parenthood to provide early abortion care. I think there were three of us in the residency that did that. We were again, the minority … most people didn’t engage with her in doing this.”
What now?
Across the country, a lot of medical schools “just do not offer comprehensive reproductive health care training, especially when it comes to abortion care,” said Haley Miller, a KU graduate working with the nonprofit Midwest Access Project in Chicago.
The program was founded in 2006 by a group of Chicago family physicians and reproductive health advocates to help medical students, doctors, nurses and other health care providers who can’t get the clinical training from their own schools or jobs.
The project helps residents and other professionals find abortion providers in 10 states who are willing to train. One is Planned Parenthood Great Plains in Overland Park.
The project was intended to assist doctors in the Midwest. But as more states impose abortion bans and restrictions, requests for help to find training are coming from across the country, and the program is looking for more providers to do the training, Miller said.
The scramble could be an inkling of things to come.
“I think that interest has stayed the same. I think what we’re actually starting to see is impact that a lot of clinics are at capacity when it comes to just providing care, and they’re not able to train as many people as they normally would,” said Miller.
“So we’re starting to see an influx of applicants come from places where they normally would be able to receive training but they haven’t been able to access it where they are, and they’re coming to us for that.
“We’re just going to keep doing what we’ve been doing and working the problem and continuing to provide training for anyone who wants to train in procedural abortion, medication abortion, family planning, contraception care.”
This month at its annual meeting, the AMA doubled down on its long-held position to “always fight government intrusion that compromises access to safe, evidence-based clinical care, including access to abortion services.”
The group plans to find expanded legal protection for patients and physicians against limits or bans that “criminalize” reproductive health services.
“I think for a lot of people who been been doing this work, we anticipated this moment for a few years now, so it hasn’t been a surprise,” said Miller. “But it definitely has been painful to now be in this moment.”
This story was originally published June 24, 2022 at 5:00 AM.
.jpg)
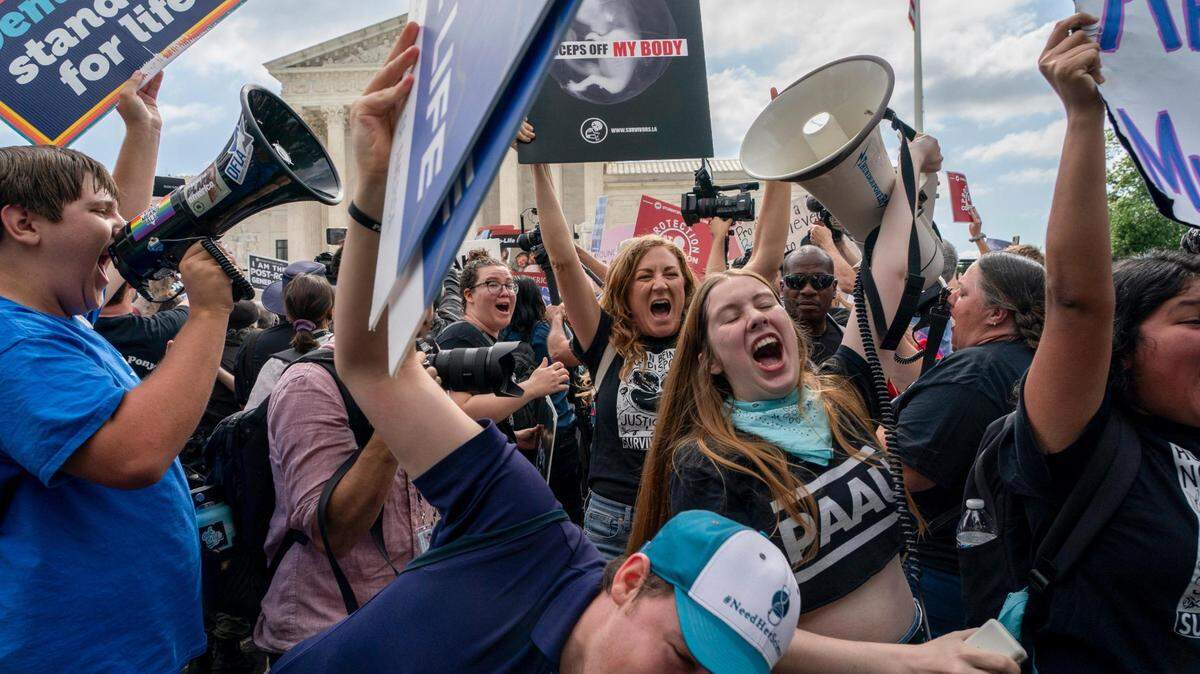



.jpg)