‘A very dangerous time’: COVID rules return as Kansas, Missouri hospitals on the brink
As the coronavirus spread across Kansas and Missouri this spring, we took extraordinary steps to slow down a new, deadly disease that raised nightmarish fears of overwhelmed hospitals flooded with COVID-19 patients.
Stay-at-home orders, mandatory business closures and mass gathering bans all bought time for hospitals to prepare and scrounge up precious supplies like ventilators and personal protective equipment. But then summer arrived, attention shifted to masks, and for a time the virus appeared under control.
The nightmare has now arrived.
Hospitals in both states are in crisis, quickly filling to capacity as the virus spreads freely through communities both big and small. Urban, suburban, rural: it’s everywhere. Each day brings numbing counts of thousands of new cases and a seemingly ever-rising tide of hospitalizations.
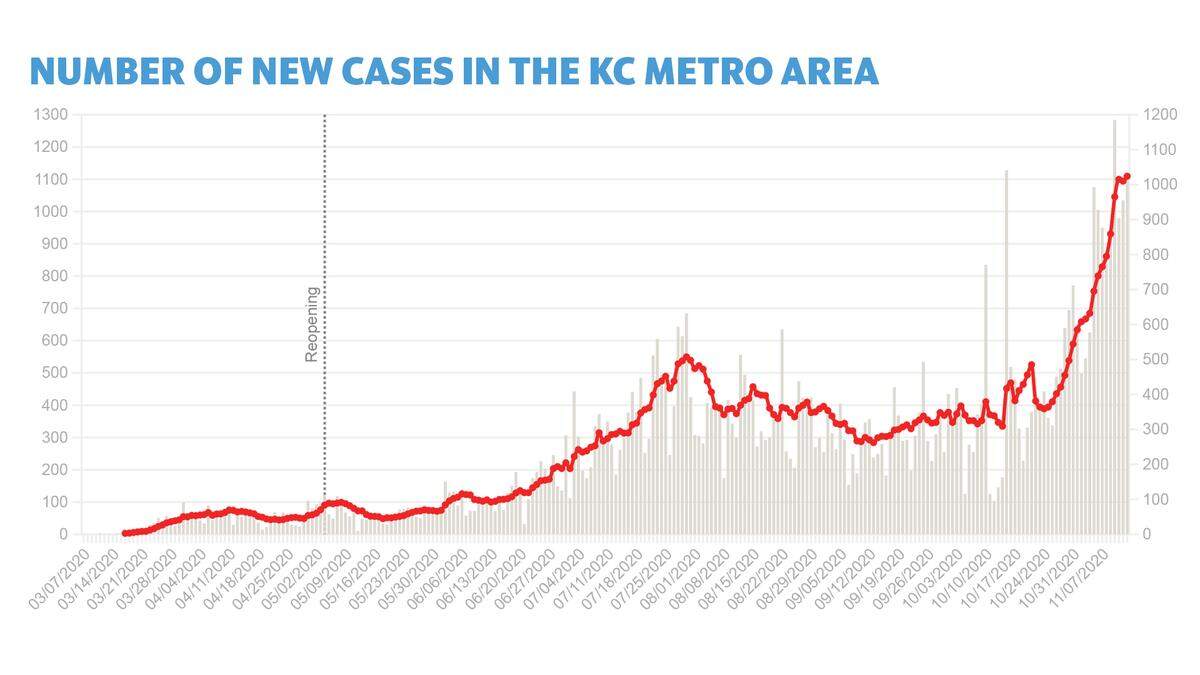
In Kansas, the seven-day rolling average of new cases in the spring never exceeded the low 300s. It’s now more than 2,400, according to data from The New York Times.
In Missouri, the average for much of the spring stayed in the low 200s. On Thursday, it was more than 4,300.
“This is a very dangerous time,” Johnson County health officer Joseph LeMaster said. “Very important to take action that will make a difference.”
But officials so far aren’t returning to the aggressive weapons they wielded to beat down the virus in March, April and May — stay-at-home orders and mandatory business closures. At least for the moment, state and local leaders are opting for lesser steps, even as the pandemic reaches its worst point ever.
Health leaders across both states, from Wichita to Kansas City to St. Louis, are pleading for action. They are focused on masks — the most effective way to slow the spread without damaging the economy — but are increasingly seeking additional measures as well.
State leaders, in turn, are making a renewed push to encourage masks but are so far not issuing new restrictions.
Kansas Gov. Laura Kelly held off on seeking a new statewide mandate after Republican leaders urged her to allow local governments to act first. Gov. Mike Parson, who has resisted statewide mandates since the start of the pandemic, continues to exhort personal responsibility while vowing to never lock down the state.
At the same time, cities and counties are starting to take more aggressive steps. Over the last week, a growing number have cut mass gathering limits, reduced bar and restaurant hours or increased fines for rule breaking.
But the scattershot effort may not be enough to avert a true catastrophe. Restrictions imposed now won’t immediately slow case numbers because of the lag between infection and symptoms. Hospitalizations and deaths could continue to surge upward for weeks even if new infections are cut substantially.
There are also limits to local action, no matter how effective. If surrounding jurisdictions don’t follow suit, especially in the Kansas City region, where tens of thousands move freely every day, the virus will continue to spread.
Health officials said more aggressive steps don’t have to be draconian.
“I don’t think we’re talking about full on lockdowns,” Wyandotte County medical officer Allen Greiner said, “but I think we’re looking at and having conversations across the Kansas City metro area about what changes we could make in terms of gathering sizes” and other restrictions.
Kansas City area hospitals have reached a tipping point where additional COVID admissions could trigger a crisis. Some hospitals, such as the University of Kansas Health System, have already begun curtailing elective procedures to free up staff and space for COVID-19 care.
Just 9% of the metro’s staffed intensive care beds — 88 beds — remained available as of Wednesday, according to data from the Kansas Hospital Association, or KHA, which tracks hospitals in the metro on both sides of the state line. South Central Kansas also reported 9% ICU availability.
Kansas City area hospitals warned this week they would soon be unable to accept transfers from rural hospitals if patient numbers keep rising. The University of Kansas Health System has already begun slowing down rural transfers and keeping patients in “alternative care” areas, such as a dialysis unit, where they wouldn’t normally be.
Across all of Kansas, 17% of staffed ICU beds were open. Missouri’s figure was slightly better at 27%, according to the Missouri Hospital Association. But the association reported all but 5% of ICU beds in northeast Missouri — three beds — were filled.
“The number of people so ill that they have to go to the hospital is nearly three times what we described as a sustainable level,” said Dr. Alex Garza, commander of the St. Louis Metropolitan Pandemic Task Force.
Even if beds are available, staffing shortages are constraining hospitals. According to KHA, 31% of Kansas hospitals on Wednesday were anticipating staffing shortages over the next week. The figure was as high as 44% in southwest Kansas.
The shortages are driven in large measure by fallout from the virus, whether it’s employees who need to quarantine or are responding to child care issues caused by closing schools, according to KHA spokeswoman Cindy Samuelson.
“As we’ve seen, community spread has increased and our people are in the community,” Samuelson said.
No statewide orders yet
Reducing community spread is the key to bringing the virus back under control, but neither Parson or Kelly are currently pushing for new statewide rules.
Parson has deferred to local authorities throughout the pandemic. He has resisted statewide mandates, especially on masks, but has also not stopped Missouri’s biggest cities from implementing their own.
Some hospital leaders last month asked Parson to take more action, including on masks, according to audio of a conference call that later leaked. Still, Parson hasn’t wavered from his approach as Missouri’s outbreak has worsened in recent weeks.
But he has acknowledged the growing strain on hospitals. “The reality of it is we can’t keep going at the pace we’re going and keep doing the same old things we’ve been doing,” Parson said Thursday.
His solution continues to be an emphasis on personal responsibility. During a news conference Thursday, Parson said he protected freedom but added it’s time for Missourians to “do our part to protect one another. No government is going to do that for you.”
Clay Dunagan, an infectious disease specialist for BJC HealthCare in St. Louis, said Parson was continuing to stick with the premise that “this is a local priority and that local governments know what’s best for their citizens.”
“Unfortunately, what we’re seeing is that’s not the case,” Dunagan said.

In Kansas, Kelly recently suggested she might call a special session for lawmakers to approve a statewide mask law, leading to a meeting with Republican leaders in late October. The governor emerged from the meeting having agreed to urge cities and counties to take action on masks first before recalling the Legislature.
In the spring, Kelly ordered non-essential businesses closed and severely limited mass gatherings statewide. In June, she agreed to a deal with lawmakers that restricted her emergency powers in exchange for an extension of Kansas’s state of emergency, which she said was vital to coordinating the virus response.
Under the deal, Kelly could order businesses closed for up to 15 days. But in order to gain approval for an extension of the state’s disaster declaration in September, the governor reassured Republicans that, “unless some mushroom cloud of coronavirus should spread all across the state of Kansas, I would have absolutely no intention of putting in a statewide stay-home order.”
Asked on Tuesday whether the time had again come for restrictions, Kelly said counties are working on those issues.
“We’re going to work in that fashion unless the data drives us to do it differently,” Kelly said.
Pressed on whether a red line exists in the data that will force a change, the governor said she wants collaboration with Republican leaders and expressed hope they can reach a consensus on what will drive the push for local mask mandates. “But I will tell you, everything is on the table. So that if we cannot come up with a consensus that will work, we will revisit that,” Kelly said.
On Friday, Kelly promised a group of Republican leaders she has no plans to shutdown businesses.
Local restrictions planned
For now, the task of deciding what restrictions are needed continues to fall to cities and counties.
Kansas City area health officers issued a joint statement Friday urging officials to take action and calling on residents to improve their mask wearing and social distancing. The statement recommended closing bars and restaurants at 10 p.m. and limiting gatherings.
Sedgwick County has ordered wedding and family gatherings limited to 100 people, or 50% of a venue’s capacity, whichever is smaller. Retail stores must tell patrons that masks are mandatory. Fines for breaking the rules have been ramped up to $500.
Douglas County cut its mass gathering limit from 45 to 15. Shawnee County dropped from 25 to 10.
In Johnson County, Kansas’s most populous county, officials had shown little interest in new limits until this week. New cases have soared since the beginning of November, however, with a record 458 reported Thursday.
Many officials are now in agreement more needs to be done. On Friday, the Johnson County Board of Commissioners voted 4-3 to approve new restrictions, including a midnight curfew for bars and restaurants, as well as a 50-person or 50% capacity limit on mass gatherings, whichever is fewer. It will be in effect Monday.
What the board approved was a weaker version of an order proposed by health officials. Commissioners voted to include broad exemptions: Shops, restaurants, bars, nightclubs, fitness centers, health care facilities, churches and funeral homes do not have to abide by the gathering limit. The restriction also does not apply to private gatherings.
Commissioner Becky Fast, who voted for the order, said she believes there hadn’t been the “public or political will” to issue new restrictions. The board has been continually split on whether to issue mandates. And while some felt the new order was a needed step, others worry that the county will continue to be hamstrung because much of the spread is originating in private parties, weddings and other personal events.
“I don’t know how much more education we can do to encourage personal responsibility,” said Commissioner Janeé Hanzlick. “We could have all kinds of regulations in place, but they’re not really going to impact these personal events.”
School districts are also coming under pressure from the spreading virus, according to Sanmi Areola, the county’s public health director. School officials in turn had grown frustrated with the lack of government action.
Shawnee Mission school district officials this past week warned families that a return to online learning was imminent, as the district faces a staffing shortage and struggles to keep up with contact tracing. Shelby Rebeck, the health services coordinator, said school nurses are working 20-hour days trying to keep up with the demands.
That’s frustrating for school administrators who say they have been told to cancel winter sports, limit gatherings and issue other protocols that they have seen no one else in the community following. Even the Johnson County Parks and Recreation department is offering the winter sports, like basketball, that health officials have said are too dangerous for schools to allow, due to a lack of social distancing indoors.
Without broader community restrictions to limit the spread of the virus, Heather Ousley, Shawnee Mission school board president, said she felt like school districts had been left on their own.
“There’s no one coming to save us,” Ousley said. “There’s no one at the federal level. There’s no one at the state level. And there’s no one at the county level.”
Kansas City Mayor Quinton Lucas said Friday the city will most likely issue a new health order on either Monday or Tuesday. It will incorporate recommendations from the metro area health officers.
Lucas said the current situation “is a huge problem.” The seven-day average for new cases in the metro has broken 1,000, rising from 455 two weeks ago.
Any additional restrictions, especially if they affect businesses, could come with an economic cost. Bill Teel, director of the Greater Kansas City Restaurant Association, said his group has had good discussions with local officials.
“We feel we’re as safe as we possibly can be,” Teel said. New limits on indoor dining, combined with the loss of outdoor dining as temperatures cool, would “hurt greatly.”
“So many restaurants right now are just kind of on the edge, they’re getting by,” Teel said.
Lucas made clear he’s well aware of the price businesses pay.
“I am someone who has said repeatedly we don’t want the cure to be any more substantial than that which is necessary to address the harm,” Lucas said. “That said, the harm is very serious. It is people dying.”
Resistance, fatigue mounting
Even if Kansas City takes action, resistance may remain in other areas. Theresa Galvin, a Jackson County legislator, said additional restrictions wouldn’t be a good idea.
“I think most of the people in Jackson County are pretty much over it, and I think if we were to go back, it wouldn’t turn out very well,” Galvin said.
In Missouri, some health departments have issued mask rules only to have county leaders not adopt them, rendering them effectively toothless. Kerri Lewis, community outreach coordinator at Johnson County Community Health, southeast of Kansas City, said the county commission didn’t endorse the department’s mask order, leading to confusion among residents.
“The breakdown is, because the commissioners didn’t choose to endorse it, folks don’t feel like they have to follow it,” Lewis said.
Pettis County Commissioner Israel Baeza said the county, situated roughly halfway between Kansas City and Jefferson City, has taken a “small-government approach.” The health department has issued a mask order but the commission hasn’t endorsed it. He said he doesn’t expect that to change.
“People are going to do — at least on this subject, people already have their mind made up what they’re going to do,” Baeza said.
Over the past week, more than 99% of tests for COVID-19 in Pettis County have come back positive, according to the Missouri Department of Health and Senior Services, or DHSS.
The wave of cases in both states is now overwhelming the ability of local health officials to investigate cases. Cole County, which includes Jefferson City, on Thursday asked COVID-19 positive residents to trace their own close contacts and reach out to them.
Dennis Kriesel, director of the Kansas Association of Local Health Departments, said his members have been asking him whether they will receive any help to keep up with disease investigations. Reaching out to every person who tests positive has become a staggering task for some departments, especially when even sparsely populated counties are posting record numbers.
Kriesel said he’s heard a number of ideas, from involving schools in investigations to having confirmed positives call their own contacts, like in Cole County. Kansas is bringing on more investigators, he said, but the volume of cases is too high to keep up.
Sedgwick County is bulking up, using federal aid to hire 52 employees to assist with testing and contact tracing as cases surge there. Not every county has the same kind of resources, however.
“On paper, we have this plan to do these individualized investigations, but we can’t do them in a timely manner now,” Kriesel said.
Kansas and Missouri are in for a long, painful winter if virus spread can’t be bent back down. Already, falling temperatures are starting to limit opportunities for outdoor dining and other activities, forcing people inside where the virus is transmitted more easily.
“At the very moment when we need to be the most vigilant … I think people are letting down their guard,” DHSS director Randall Williams told lawmakers last week.
A vaccine offers some hope. Williams said some healthcare workers in Missouri could begin receiving one in December, which holds the potential to alleviate staffing shortages.
Even the rosiest predictions don’t anticipate enough doses for the general public until April, however. Kriesel said health departments are expecting case numbers to get worse.
“The forecast is relatively bleak,” he said.
Contributing: Katie Moore and Kelsey Landis
This story was originally published November 15, 2020 at 5:00 AM.
