‘Totally in the dark.’ National shortage of COVID-19 tests hamstrings Kansas, Missouri
Kansas, Missouri and other states have had to limit coronavirus testing to people with severe symptoms because of the national shortage of test kits, but health policy experts say broad-based screening is critical to understanding and containing the disease.
Kansas Secretary of Health and Environment Lee Norman has had to ration COVID-19 testing in populous Johnson County, the jurisdiction with the most positive cases in the state, because of the overall shortage.
In a teleconference with Sen. Jerry Moran on Monday night, Norman described the ideal scenario, one with enough tests that health officials could search for patterns of infection and try to identify asymptomatic carriers.
“What I would like to look at is not only how do we manage a disease, in this case an epidemic, but what do we know about the communities? Do we do community surveillance of well people just to find out where does the virus live?” Norman said. “Are there asymptomatic people that carry it? Are there people who shed the virus? And we have not been able to do broader community surveillance like we would like to.”
Norman announced last week that the Kansas was in danger of running out of test kits. He said the state narrowly avoided that calamity with a truckload from the national stockpile. But as quickly as the tests are offloaded in Topeka, he noted, they’re sent back out as more Kansas counties screen for the virus.
The state has adjusted its testing protocols to ensure that hospitalized patients and mission-essential health care workers get priority. But the restrictions mean that the daily update on positive cases is far from a complete picture of the virus’ spread in Kansas.
“Until we do more community surveillance we aren’t really going to know the prevalence of the disease,” Norman said.
Moran, the Kansas Republican who held the joint teleconference with Norman, praised private sector efforts to ramp up test kit production and noted that the Food and Drug Administration has shortened its approval process, which means more kits will become available every day.
But Moran acknowledged frustration that the national kit shortage was affecting local health officials’ decisions about who can be tested.
“I’ve been concerned for a long time that the answer of who should be tested is based upon how many tests are available. That’s necessary. We started at a woefully inadequate supply and we can’t use them where they aren’t the highest priority,” Moran said.
“But I do want to know what the CDC would say if we had more tests what should be the protocols for who should be tested and when.”
Sitting around wondering
In meantime, several Kansas City area residents are grappling with uncertainty about symptoms that aren’t considered serious enough to merit testing.
Magan Gutierrez, 43, a Cass County resident, said that she and her husband developed fevers and coughs after going on a Carnival cruise in late February. She then saw a news report about a person in Ohio on the same cruise who tested positive for coronavirus.
She called Missouri’s state hotline, her primary care doctor, the Cass County Health Department and Belton Regional Medical Center in hopes of getting tested.
“They said even if they wanted to test me, they don’t physically have any (test kits),” she said of her conversation with Belton in early March.
She and her husband went into quarantine for 14 days based on the guidance of the Missouri hotline, but she’s been fretting that she may have spread the disease before she went into quarantine. She’s the primary caregiver for her mother who suffers from chronic obstructive pulmonary disease.
“Sitting around every day wondering if I introduced the virus that would kill my mom… and who else I might have exposed,” Gutierrez said.
Torey Crawford, 39, another Cass County resident, said he experienced uncontrollable coughing and shortness of breath when he returned home from Germany on March 2.
Both his local health department and his primary care doctor with the Veterans Administration said he wasn’t eligible for a test because at that point Germany wasn’t deemed a high risk country.
“Maybe I was one of the ones that brought it back, but I was unable to get it tested from the beginning,” Crawford said.
Rachel Johnson, 38, a Johnson County resident, said that every member of her family has developed a fever or cough since her husband returned from a February trip to Seattle, including her 9-year-old daughter who can’t get approved for a test despite having a fever for 12 days.
“I’m not mad at the doctors. They are doing everything they can. I am frustrated that there is no way to implement best practices because there are no tests available,” she said.
‘We have no idea’
Former Kansas Gov. Kathleen Sebelius served as President Barack Obama’s secretary of Health and Human Services during the 2009 outbreak of H1N1, sometimes more commonly called swine flu.
She recalled how the Centers for Disease Control and Prevention produced an H1N1 test within two weeks of its discovery in the U.S. and that the U.S. government quickly became an international supplier of the test kits, distributing 1 million worldwide.
Sebelius attributed the shortage to a breakdown at the CDC and President Donald Trump’s administration’s refusal to buy already-available COVID-19 tests from the World Health Organization.
As a consequence, she said, Kansas and other states have had to take extraordinary measures, such as closing schools and restricting public gatherings because of the threat that asymptomatic carriers will spread the deadly virus.
“A lot of what we’re doing here is desperately try to catch up,” Sebelius said.
“We have no idea how many asymptomatic people there are in the country,” Sebelius said. “What we should be doing ideally is testing broadly in population centers to see how many asymptomatic people are in the population.”
Sebelius said until there are enough tests for public health officials to identify patterns, policymakers will be “totally in the dark” about the spread of the disease.
Stephen Morse, an epidemiologist who teaches at Columbia University’s Vagelos College of Physicians and Surgeons in New York, made a similar point last week.
“The normal response if we were able to do broad testing is to test so you know where to concentrate your resources, but we don’t have the capacity to do testing on that scale so we had to limit it. I think we’ve had to limit it too much in my opinion,” Morse said. “It’s a question of scarce resources and allocating them.”
The CDC did not respond to questions about the test kit shortage and how it was affecting containment efforts.
Deborah Birx, the response coordinator for the White House Coronavirus Task Force, said at a news conference Tuesday that the U.S. was accelerating testing capacity at a record rate.
“We now have 370,000 tests that have been done. The majority of those - over 220,000 in the last eight days, which, those of you who have been tracking the South Korea numbers, put us equivalent to what they did in eight weeks that we did in eight days,” she said.
Trump downplayed concerns about about the need for more tests in the Midwest during Wednesday evening’s news conference. He contended that broad testing isn’t needed in the heartland in the same way as coastal states with more positive cases, such as New York and California.
“We don’t have to test the entire state in the Midwest. I think it’s ridiculous. We don’t have to do it,” Trump said.
Shifting protocols
But even as more tests become available, health departments and hospitals will face difficult decisions about testing because of the limited supply of essential medical equipment.
Kayla Parker, a spokeswoman for the Jackson County Health Department, pointed to the U.S. shortage of protective personal equipment as a reason to restrict testing to only serious cases.
“Healthcare workers must wear personal protective equipment (masks, gowns, goggles, and gloves) to perform the test. To preserve supplies, we are working with healthcare providers to test people only when necessary,” she said in an email.
Parker argued that that testing is only necessary in cases where it’s likely to affect treatment.
“For mild to moderate symptoms, a test result does not change the treatment plan to stay home and away from other people until symptoms resolve,” she said.
Steve Stites, the chief medical officer for the University of Kansas Health System, said hospitals burn through large amounts of protective gear and other resources while waiting for patients’ test results regardless of whether they end up testing positive for COVID-19.
“When that happens, you can’t preserve that equipment for the real patient who comes in with it,” Stites said. “So the patient is sitting in the hospital for three, four or five days waiting on results for a test. That was a huge limiting factor.”
Testing by private labs has helped relieve some of the burden from state and county health departments.
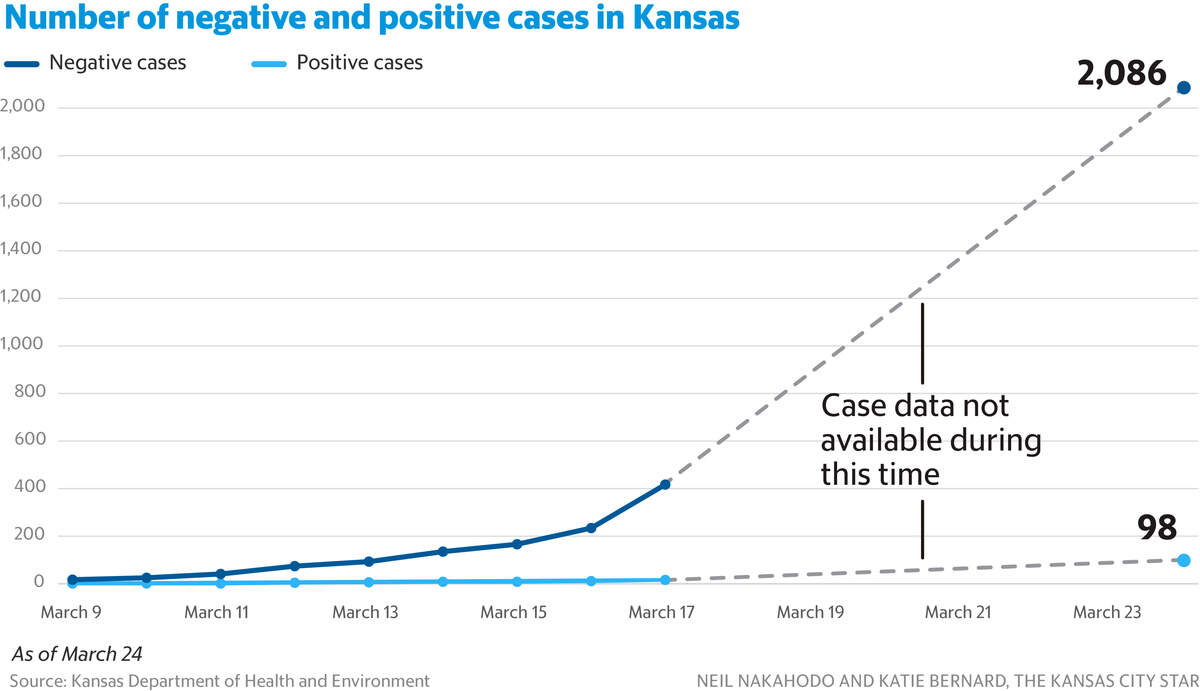
As of Wednesday afternoon, Kansas had 127 positive cases—with 77 coming from private lab tests. The state reported 2,360 negative cases, a figure that includes people tested by both the state and private labs.
Missouri officials estimate that private labs have tested thousands of people, but the state is not tracking their negative tests. In Kansas City, Missouri, 24 of the 29 positive cases have come from tests done by private labs as of Tuesday.
The state labs are testing at a rate of less than 100 people a day — 660 through Tuesday morning with about 8 percent testing positive. Missouri had 356 cases as of Wednesday afternoon.
“Every governor wishes we had more tests on hand. But unfortunately the supply in the United States are not what they should be,” Missouri Gov. Mike Parson, a Republican, said Tuesday.
Missouri adjusted its testing protocols this week based on CDC guidelines. Tests are available for hospitalized patients with COVID-19 symptoms, symptomatic residents of senior living facilities, the immunocompromised who are at higher risk for poor outcomes and health care workers and others who show symptoms after contact with a suspected COVID-19 patient.
Randall Williams, the director of the Missouri Department of Health and Senior Services, said the changes to the testing policy give clinicians more discretion to decide who gets tested.
The Star’s Jason Hancock, Steve Vockrodt and Allison Kite contributed to this report.
This story was originally published March 25, 2020 at 1:47 PM.

