Kansas City area hospitals are short on ventilators. Here’s why that matters
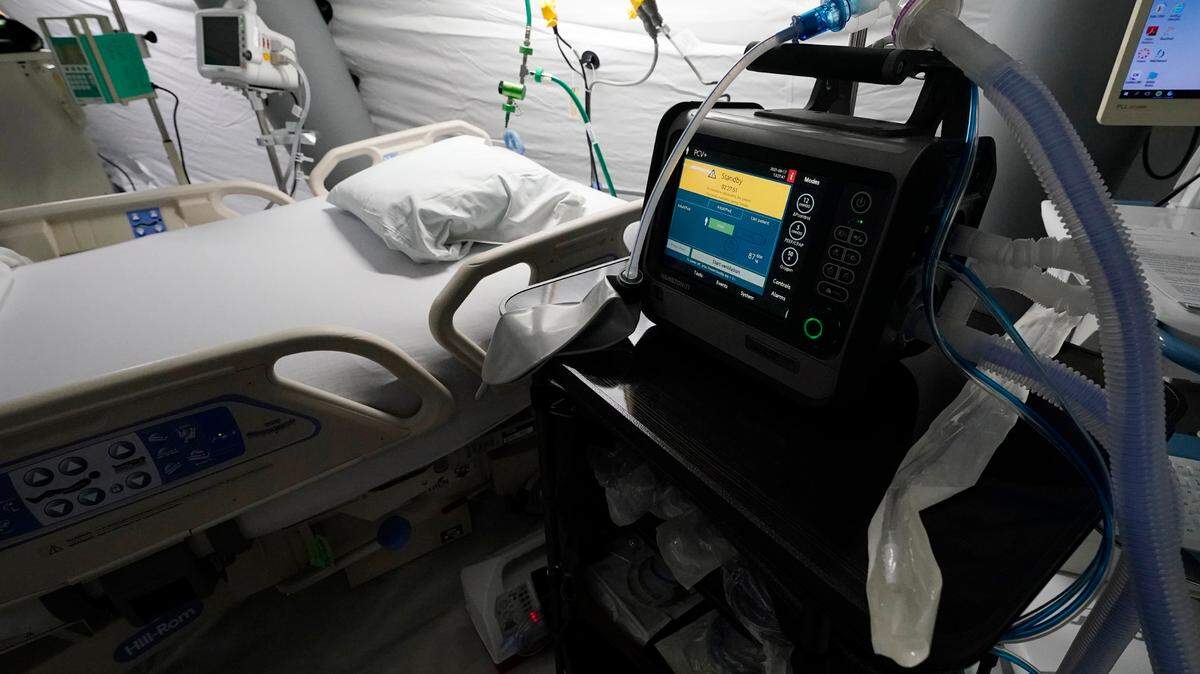
Intubation via a ventilator has become a widely recognized symbol of severe COVID-19 over the past two years of the pandemic.
Some hospitals around Kansas City are facing a shortage of the devices reminiscent of early days of the pandemic, according to five area hospital officials that spoke at a briefing held by the University of Kansas Health System on Wednesday, Jan. 12.
The doctors also said that this machine is only one of the tools used to treat serious illness — and sometimes the specific kinds of ventilators they have in house may not be up to the job of treating a severely ill COVID-19 patient.
Here’s what to know about ventilators in local hospitals.
Are local hospitals running low on ventilators?
Yes and no. The recent rise in COVID-19 cases around the Kansas City area has been straining hospitals to their limit, forcing some to request extra ventilators. The states of Missouri and Kansas both have a strategic supply of ventilators to deploy to hospitals in need.
“Our ventilator situation has been a bit tenuous this week,” said Dr. Lisa Hays, Chief Medical Officer at AdventHealth Shawnee Mission. “I got an emergency call Saturday night from our chief nursing officer that we were down to one ventilator. I came in and assessed the situation and we were able to procure seven more ventilators, and those started coming in yesterday.”
Liberty Hospital has also tapped into this resource, acquiring five extra ventilators over the weekend. Doctors say that one reason they request the extra machines from the state, or share them between associated hospitals, is that some ventilators already in their facilities aren’t sufficient to treat COVID patients.
“We have many ventilators in house, but not all of them are able to handle the high oxygen requirements that our COVID patients require,” said Hays.
Some types of ventilators are strong enough to use on COVID-19 patients, while some are less powerful and may be unfamiliar to hospital staff, added Dr. Lewis Satterwhite, a critical care physician at The University of Kansas Health System.
“Not all of them are created equally, and not all of them are able to support the very, very sick people with bad lung injury,” he said. “It just adds to the stress on the system.”
Are ventilators a good metric of how severe the COVID crisis is?
Not always.
“Some people have been tracking the number of ventilators used in the pandemic as the only indicator of the severity of the disease. That’s not a great metric to follow,” said Dr. Sam Antonios, Chief Clinical Officer at Ascension Via Christi Health in Wichita. “Our use of ventilators has declined because we actively put people on high-flow oxygen [machines] and other tools that don’t necessarily intubate patients.”
That means that statistics showing ventilator availability often don’t paint a complete picture of the situation inside hospitals. The number may look higher than it is because it includes subpar ventilators, or it may really be high because other machines are better suited to patients’ needs at the time.
That doesn’t mean that patients aren’t sick or that hospitals aren’t overwhelmed— just that some machines work better than others in different situations.
What other factors may tell us more about the severity of this wave and the strain on hospitals?
Hospitalization rates themselves, alongside case numbers and death rates, are a better way to gauge the severity of the latest wave.
Death rates appear to be rising in the Kansas City area, and case numbers are still skyrocketing. Recent data collected by The Star shows that an average of 3,554 have gotten sick with COVID-19 every day for the past seven days.
Check hospital occupancy in your area on this interactive map.
Do you have other questions about staying safe from COVID-19 in the Kansas City area? Ask our Service Journalism team at kcq@kcstar.com or fill out the form below.
.jpg)