STDs are on the rise. KC med students have treatment plan, but Kansas law is a hurdle
Kansas City medical student Mianna Armstrong was on the front lines of the fight against sexually transmitted diseases.
With chlamydia and gonorrhea on the rise locally and nationally, the Centers for Disease Control recommends that as soon as doctors and nurses diagnose someone with an STD, they write prescriptions not only for the patient but also for that person’s sexual partners, sight unseen if necessary.
But that was virtually impossible at the community clinic in Joplin where Armstrong was working last year as a third-year med student. Patients came there from four states, filled their prescriptions in four states and had partners in different states.
“Every state has different rules and laws about what’s allowed,” Armstrong said.

Thanks in part to her experiences and research, the American Osteopathic Association discussed recommending that every state legalize “expedited partner therapy,” so both STD patients and their sexual partners can get prescriptions, even if the doctors or nurses haven’t personally examined the partners.
Armstrong, along with her Kansas City University of Medicine and Biosciences classmate Megan McMurray and their teacher John Paulson, published a paper in January about rising STD rates that mentioned that expedited partner therapy is legally limited in seven states — including Kansas and Oklahoma — and effectively banned in Kentucky and South Carolina.
The practice is allowed in Missouri, but even so, health officials there are treading carefully.
The American Osteopathic Association drafted a resolution this summer to endorse legalization of expedited partner therapy in all states, in line with the CDC recommendations. It was later amended to just advocate for doctors to use expedited partner therapy when the state law allows.
“We can advocate for (it), as an organization,” the association’s president, Bill Mayo, said during a recent visit to KCUMB. “But we cannot draft legislation and pass laws.”

Still, Mayo said that as a KCUMB grad himself, he was proud of the research Armstrong and McMurray had done and that it would inform state osteopathic associations’ positions on legislation.
Public health officials around the country are trying to figure out how to reverse a steady and persistent increase in STDs. In Oregon they’ve been going door-to-door to warn sexual partners of those who have been diagnosed. But that can be dangerous to those workers and difficult for health departments that, by and large, have had reduced or stagnant funding over the last decade.
Experts agree that the best case scenario is for everyone exposed to an STD to visit a physician with whom they have an established doctor-patient relationship.
That’s not always realistic, though, and in cases where patients diagnosed with STDs still have good relationships with their partners, enlisting those patients to bring their partners antibiotics can be the quickest, easiest way to prevent the cycle of reinfection and stop illnesses from spreading.
Missouri law explicitly allows licensed doctors to use expedited partner therapy to treat chlamydia and gonorrhea, the two conditions for which the CDC recommends it.
But Kansas law is silent on the practice specifically and murky on whether doctors and pharmacists are allowed, in general, to prescribe and dispense drugs to patients they haven’t seen. A CDC analysis of state laws determined the practice is “potentially allowable” in Kansas, but Armstrong said doctors need more clarity because they’re justifiably concerned about legal liability.
Kansas law essentially leaves it up to the state medical board to decide whether the practice meets appropriate standards of care or if it could be cause for a physician’s license to be sanctioned.
Mayo, who serves on the medical board in his home state of Mississippi, said that given the CDC recommendations, doctors could make a good case to the board that they did the right thing. But if, for example, a patient’s partner had an allergic reaction to an antibiotic and was harmed, the partner could make a complaint to the board.
“One of the biggest fears physicians have is to be called before the board of medical licensure,” Mayo said. “You’ve spent four years in college, four years in med school, three to seven years in residency training in addition to fellowships after that if you did those, and all it takes is the strike of one pen to take away your license.”
The Kansas City Health Department has wanted to use expedited partner therapy for awhile, said Tiffany Wilkinson, manager of its division of communicable disease prevention. But the department has been taking its time to make sure it has the legal authority, its physicians are on board and it has the right policies for when the practice should be used.
“We’ve been looking at this for a number of years actually,” Wilkinson said. “It’s definitely one of the tools in the toolbox we’ve been wanting to move forward with.”
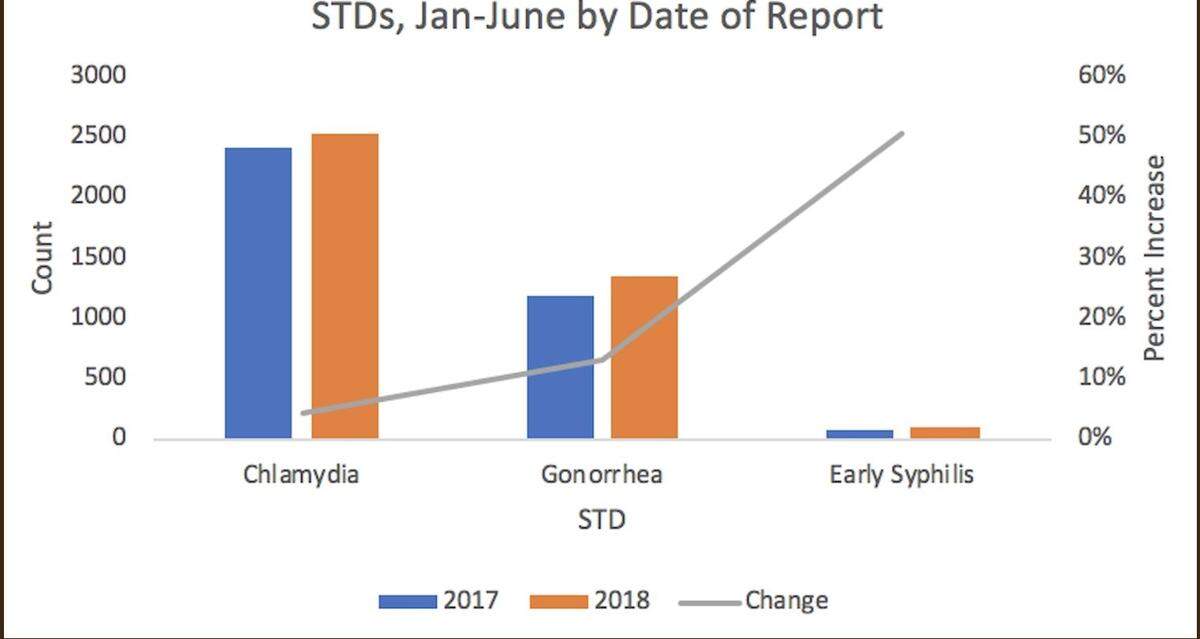
According to the Kansas City Health Department, cases of chlamydia were up about 10 percent in the first six months of 2018, versus the same time period last year. Cases of gonorrhea climbed almost 20 percent.
Wilkinson said the department prefers in-person injections for gonorrhea, but has been working with the University of Missouri-Kansas City School of Nursing to develop policies for treating partners’ chlamydia and plans to roll out a pilot program soon.
“Obviously if it’s somebody we think we can get in, we prefer to have them come in and be examined by our staff,” Wilkinson said. “(But) the cases continue to be rampant in this community, and we’re just trying different things to address chlamydia.”
The stakes are particularly high for women.
The American College of Obstetricians and Gynecologists is one of several major medical groups that recommend using expedited partner therapy, because women, even if they’re being treated themselves, are particularly susceptible to reinfection from male partners, and STDs can cause problems with their fertility and pregnancies.
Armstrong cites a lot of potential reasons for the increase in STDs, locally and nationally.
Better diagnostic tools probably have doctors identifying them more often than they used to. Several contraceptive methods are taking the place of condoms — which, unlike other options, prevent STDs as well as pregnancy. And while funding for STD prevention programs is up, funding for STD screenings is down.
The paper authored by Armstrong, McMurray and Paulson determined that physicians have to get better at interviewing patients about their sexual histories and screening them for STDs. But more widespread use of expedited partner therapy could help once those patients screen positive.
Armstrong said Congress could standardize the patchwork of state laws by enacting federal legislation allowing expedited partner therapy.
“It can give people who don’t have access to health care access to the medications they need to treat the infection,” Armstrong said. “If somebody’s working day shift and they’re in a rural community, they don’t have access to health care outside of regular hours, they can’t get time off work, they can’t get to a clinic because of transportation issues. There’s just so many issues that affect patient care that if we can just do the expedited partner therapy, then it can prevent that cycle of re-infection.”
This story was originally published September 18, 2018 at 5:30 AM.